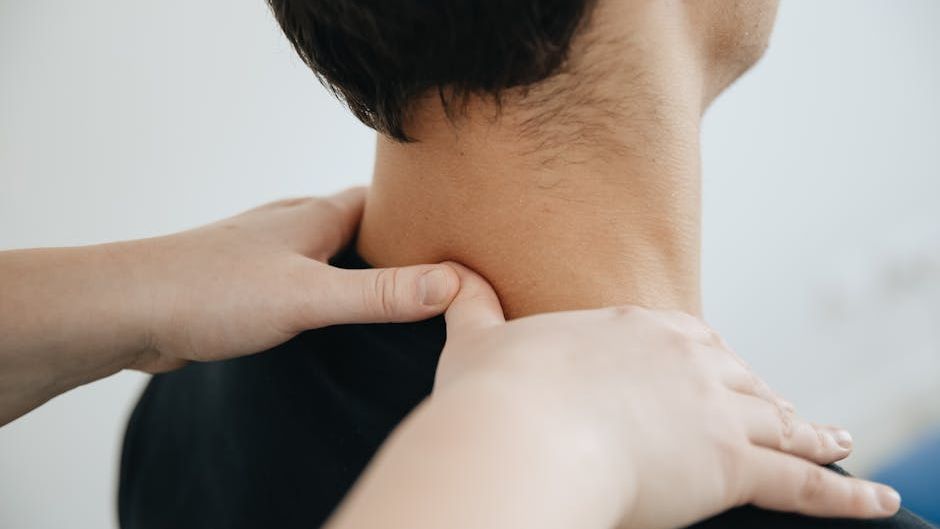
What the Vagus Nerve Actually Is
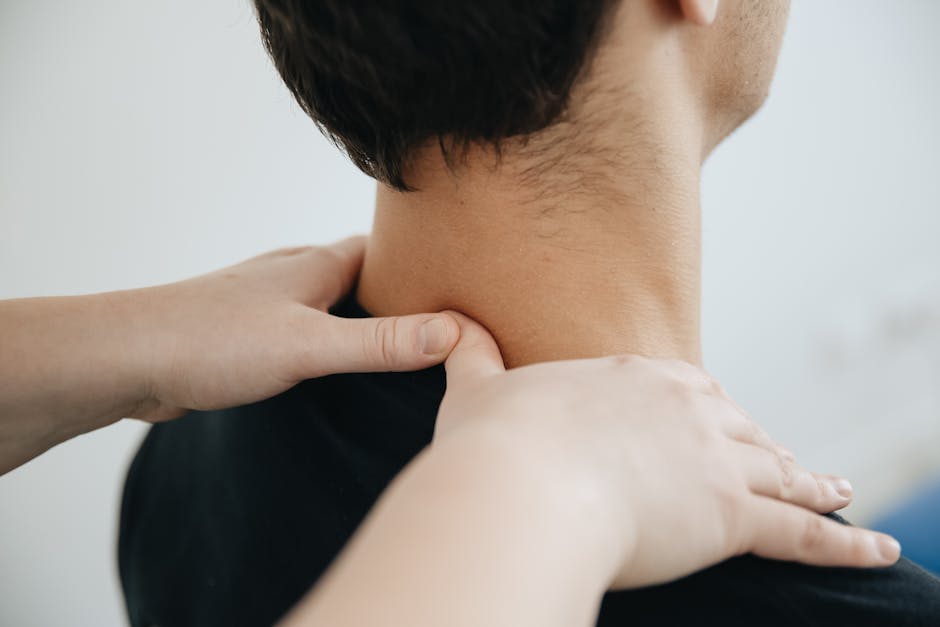
The vagus nerve is the longest cranial nerve in the human body, stretching from the brainstem all the way down to the abdomen. Its name comes from the Latin word for “wandering,” which perfectly describes how it meanders through the neck, chest, and gut, touching nearly every major organ along the way.
This single nerve carries roughly 80 percent of the sensory information flowing between your body and your brain, making it one of the most information-dense structures in your entire nervous system. Functionally, it is the cornerstone of the parasympathetic nervous system, the biological counterforce to the stress-driven sympathetic state most modern people spend too much time in.
The vagus nerve is a vital link between mind and body, regulating everything from heart rate and digestion to mood and immune function. That breadth of influence is precisely why stimulating it, even gently, can produce effects that reach well beyond the neck itself.
Why Cortisol Is the Real Problem

An acute stress response is based on the complex interplay between different pathways. It is initiated by stress centers in the central nervous system and communicated to the body by the activation of the hypothalamic-pituitary-adrenal (HPA) axis and the sympathetic nervous system. Increased HPA axis activity leads to the secretion of cortisol, one of the most important stress markers.
Cortisol is the body’s primary stress hormone, and chronically elevated levels are linked to impaired immunity, disrupted sleep, muscle breakdown, and increased cardiovascular risk.
Physical or mental imbalance caused by harmful stimuli can induce stress to maintain homeostasis. During chronic stress, the sympathetic nervous system is hyperactivated, causing physical, psychological, and behavioral abnormalities. The modern lifestyle, with its unrelenting deadlines and digital noise, keeps many people in exactly this hyperactivated state.
The Anatomy That Makes Neck Massage Work
The vagus nerve runs from your brainstem, through your neck, down to your chest, and all the way to your abdomen. In the neck, it travels within the carotid sheath right next to the sternocleidomastoid muscle, the ropey muscle on the side of your neck.
When mechanical pressure or vibration is applied to the soft tissues of the neck, it activates mechanoreceptors, which are sensory nerve endings embedded in the skin, fascia, and muscle that detect touch, pressure, and movement. These receptors, particularly the large-diameter A-beta fibers, send signals directly to the brainstem via the afferent branches of the vagus nerve itself and adjacent cervical sensory pathways.
Most people think of the vagus nerve as something the brain uses to control the body. In reality, 80 percent of its fibers run toward the brain, not away from it. This means physical stimulation at the neck isn’t just relaxing muscles – it’s sending real-time safety signals directly into your central nervous system.
What the 2025 Research Actually Found

Activation of neurons in the nucleus of the solitary tract by transcutaneous auricular vagus nerve stimulation may activate inhibitory pathways projecting to the hypothalamic paraventricular nucleus, thus inhibiting corticotropin-releasing hormone release and improving glucocorticoid dysfunction in chronic inflammatory conditions.
Salivary cortisol levels during a stress test were significantly lower during vagus nerve stimulation compared to sham conditions. This 2025 study, published in Physiological Reports, provides some of the clearest mechanistic evidence yet that stimulating vagal pathways can directly suppress the cortisol stress response.
The study demonstrates that transcutaneous vagus nerve stimulation acutely inhibits the salivary cortisol response to stress. Even though a patient case study suggests it also suppresses the HPA axis chronically, this incidental finding needs to be confirmed by properly powered studies. The science is promising, but it’s still evolving.
The Role of the SCM Muscle
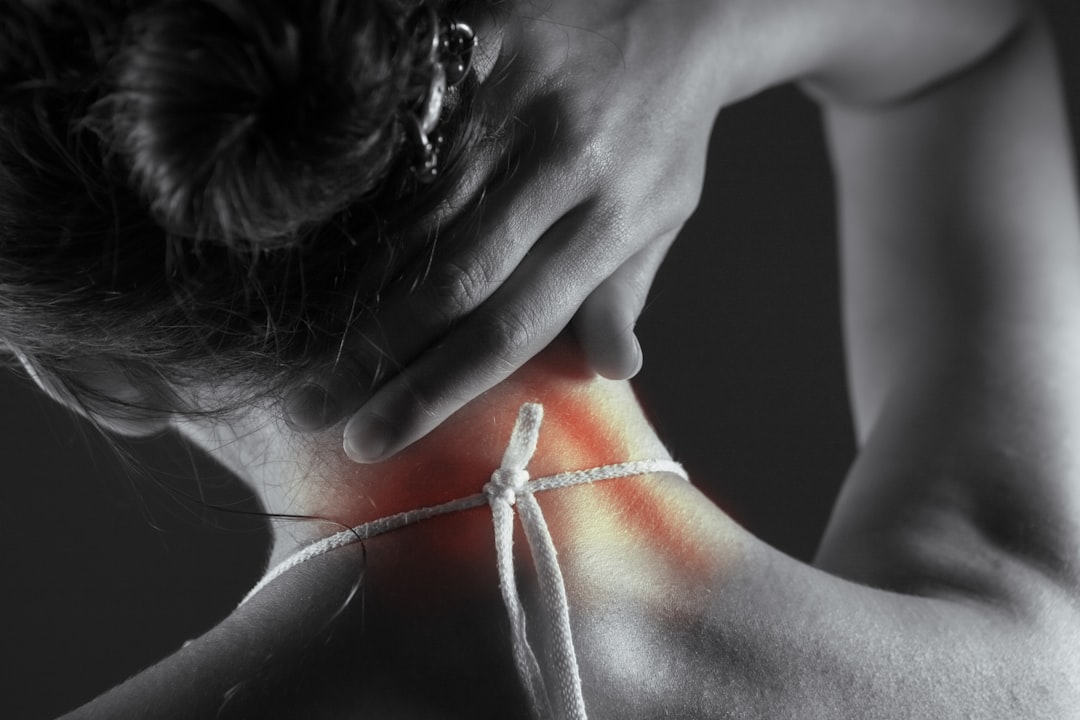
In the neck, the vagus nerve travels within the carotid sheath right next to the sternocleidomastoid muscle. Forward head posture, mouth breathing, chronic stress, and airway resistance can create tension in this area. That tension can compress or irritate the vagus nerve and surrounding fascia.
The sternocleidomastoid muscles sit on the sides of the neck. The SCM may be chronically tight or loose, adding to the stress state in your nervous system. For most desk workers, this muscle is almost perpetually braced.
One overlooked reason why calming techniques fail is mechanical tension. Releasing tension in the SCM muscle and surrounding fascia can help free the vagus nerve to do its job. Think of it less as “massaging a nerve” and more as clearing the environment around a nerve so it can transmit properly.
How to Do the 5-Second Neck Massage Correctly
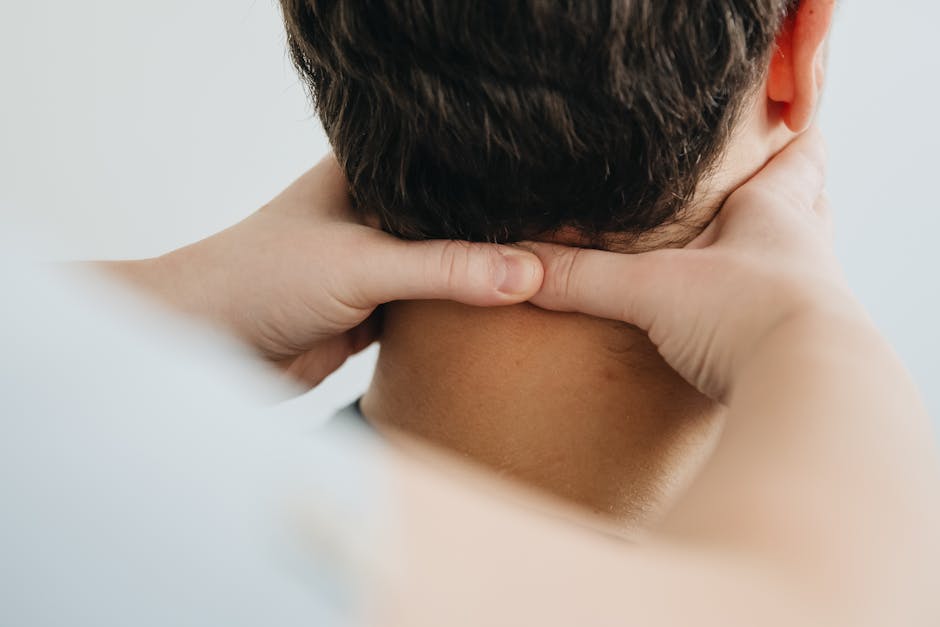
Using your fingertips or the palm of your hand, apply gentle pressure to the areas where the vagus nerve is located. Begin at the base of the skull and move down towards the sides of the neck, applying light pressure in a circular or stroking motion.
Gently place your fingers on the SCM. Apply light pressure while rotating your head slowly side to side. Move your fingers from the center of the muscle up towards the mastoid and down toward the sternum. Keep the pressure light – this is not a deep tissue massage.
Technique, pressure, and placement are critical – unfocused rubbing does far less than a deliberate, anatomically-informed approach. Even within a 5-second window, staying intentional about where you place your fingers makes a measurable difference.
Pair It With Breathing for a Stronger Effect
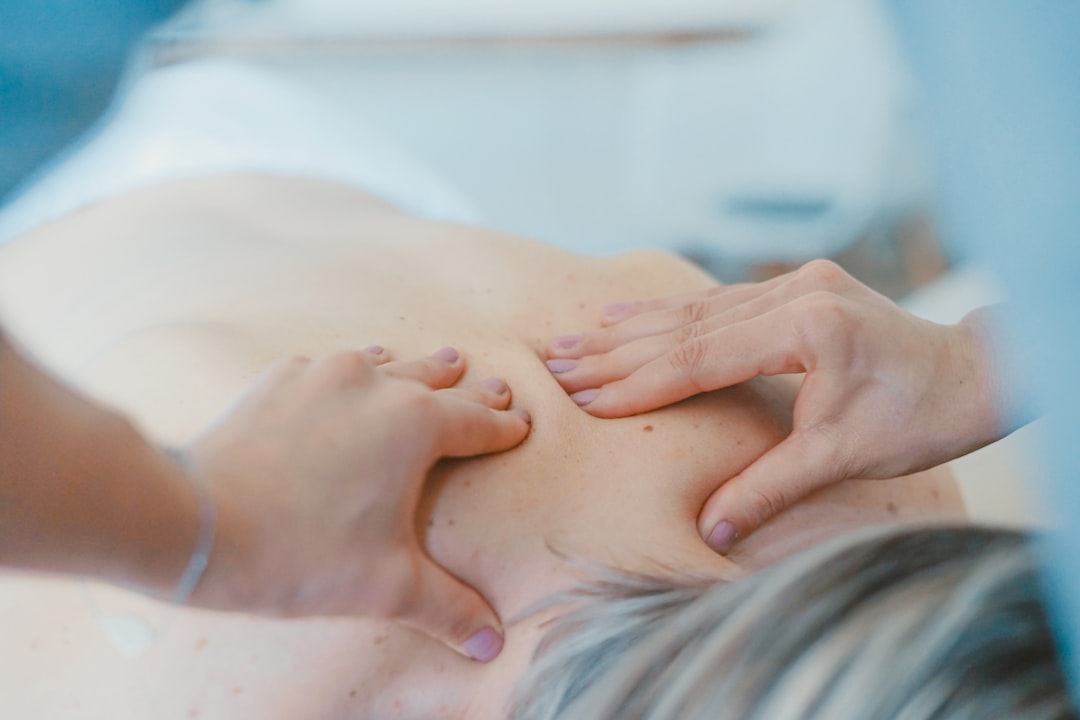
Inhale for four seconds, then exhale for six seconds. When you exhale longer than you inhale, it tells your vagus nerve that you’re not in danger, which allows it to relax. Pairing this breathing pattern with the neck massage creates a compounding effect on the parasympathetic nervous system.
Even single sessions of as low as 2 minutes of slow breathing resulted in increased HRV, suggesting breathwork is accessible, cost-effective, and convenient. Combined with targeted neck contact, the calming signal to the brain arrives through two separate channels simultaneously.
As you massage the vagus nerve area, focus on relaxation and deep breathing. Take slow, deep breaths in through the nose and out through the mouth to enhance the calming effects of the massage and activate the parasympathetic nervous system.
What Massage Does to Cortisol Levels
A landmark review published in the International Journal of Neuroscience by Tiffany Field and colleagues at the Touch Research Institute found that massage therapy consistently reduced salivary and urinary cortisol levels, often by 20 to 30 percent, across a wide range of populations and conditions.
Research shows that targeted cervical massage reduces salivary cortisol and improves heart rate variability, two gold-standard markers of stress and recovery. These aren’t isolated findings. They appear consistently across different methodologies and populations.
Vagus nerve stimulation has been shown to decrease cortisol levels, promoting a reduction in stress and anxiety. This reduction in cortisol levels can lead to improved mood, better sleep, and reduced feelings of stress and tension.
HRV as Your Progress Indicator

Heart rate variability is a non-invasive biomarker of vagal tone and autonomic flexibility. A reduced HRV has been associated with cardiovascular diseases, hypertension, inflammation, and mental health disorders.
Stress and psychosomatic disorders including anxiety, depression, chronic pain, fibromyalgia, and insomnia are consistently associated with reduced HRV, characterized by diminished vagal tone and altered autonomic ratios. These changes underscore autonomic imbalance and heightened sympathetic dominance.
A 2024 study found that 10 minutes of daily neck massage increased HRV by 15 percent, reducing anxiety in 70 percent of participants. If you use a wearable device that tracks HRV, this metric gives you a tangible, real-time window into how well your vagal tone is improving over days and weeks.
Who Should Be Careful and Why
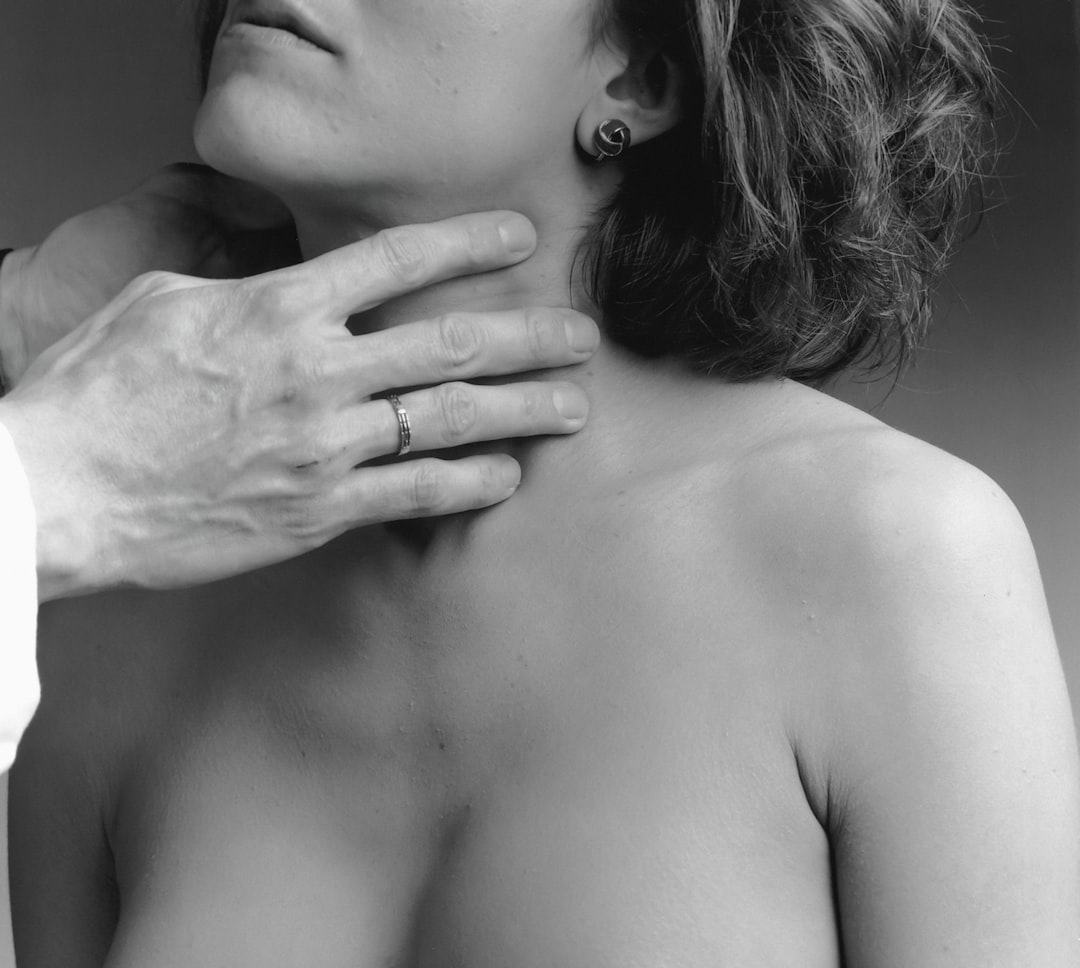
You cannot press the vagus nerve directly because it sits too deep inside your body. However, pressing certain neck areas like the carotid sinus can be dangerous, potentially causing blood pressure drops, fainting, or worse. This is not a reason to avoid the practice entirely, but it is a reason to be deliberate about where exactly you place pressure.
For most healthy individuals, gentle vagus nerve massage techniques performed at home are considered safe when done correctly and with moderate pressure. However, people with certain conditions, including carotid artery disease, heart arrhythmias, or a history of fainting, should consult a physician before attempting any form of vagus nerve stimulation.
Technique, pressure, and placement are critical. Always stay on the lateral side of the neck, keep your pressure light, and move with the SCM muscle rather than pressing straight down into the neck. If anything feels uncomfortable or causes dizziness, stop.
Conclusion
The idea of a 5-second neck massage as a genuine stress intervention isn’t wellness hype. It’s grounded in a converging body of research on vagal anatomy, cortisol regulation, and the measurable effects of targeted touch on the autonomic nervous system. The technique works best when done with correct placement, light deliberate pressure, and slow breathing as a companion.
What makes this approach worth incorporating into daily life isn’t that it’s a magic fix. It’s that it’s fast, free, anatomically sound, and backed by a growing body of physiological evidence. In a world where stress rarely waits for a convenient moment, having a tool that takes five seconds and works from the inside out is genuinely useful.
The vagus nerve has been regulating your body’s stress responses your entire life. The reset, it turns out, was always within reach.