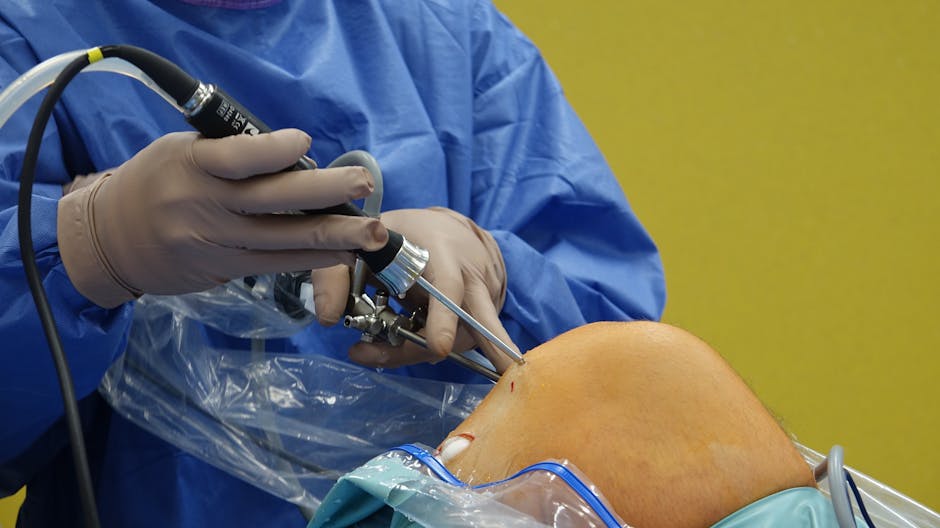
Daily Impact of Meniscus Tears on Patients (Image Credits: Pexels)
For patients grappling with knee pain from meniscus tears, the decision to undergo surgery often promises quicker recovery and lasting relief. A rigorous 10-year study, however, paints a different picture. Those who received the standard procedure ended up with diminished knee function and heightened osteoarthritis compared to individuals assigned to a sham operation. This finding challenges long-held assumptions about one of the most frequent orthopedic interventions.
Daily Impact of Meniscus Tears on Patients
Meniscus tears affect the knee’s cartilage, disrupting stability and cushioning during everyday activities like walking or climbing stairs. Many patients experience persistent pain and swelling, prompting them to seek surgical solutions. Partial meniscectomy, which removes the damaged portion of the meniscus, has become a go-to treatment due to its minimally invasive nature and rapid initial recovery.
Doctors typically recommend this surgery for active individuals or those whose symptoms do not improve with rest and physical therapy. The procedure aims to alleviate discomfort by trimming away torn tissue. Yet the long-term consequences remained unclear until recent extended research provided clearer insights.
Design of the Landmark Sham Surgery Trial
Researchers designed the study to rigorously test the true value of partial meniscectomy. Participants with confirmed meniscus tears were randomly divided into two groups. One underwent the actual surgery, while the other received sham surgery – a placebo procedure involving incisions and manipulation but no tissue removal.
This approach eliminated bias from patient expectations or surgeon skill variations. Both groups followed similar post-operative rehabilitation protocols. Tracking continued for a full decade, allowing evaluation of sustained effects on knee health and daily function.
Striking Long-Term Results Favor Non-Surgical Path
After 10 years, the surgery group fared worse across key measures. Knee function declined more sharply in those who had the partial meniscectomy, limiting their ability to perform routine tasks without pain or instability. Osteoarthritis progressed at a faster rate, evidenced by greater joint degeneration.
In contrast, the sham surgery patients maintained better overall knee performance. Their osteoarthritis developed more slowly, preserving mobility over time. These differences held despite initial similarities in age, tear severity, and baseline symptoms.
| Outcome Measure | Surgery Group | Sham Group |
|---|---|---|
| Knee Function | Poörer after 10 years | Better preserved |
| Osteoarthritis Severity | Worse progression | Slower development |
Why Surgery Might Accelerate Joint Decline
Removing meniscus tissue alters the knee’s natural shock absorption. This change places extra stress on surrounding structures, potentially hastening cartilage wear and osteoarthritis onset. Patients in the surgery arm experienced these effects cumulatively over the decade.
Sham participants, spared the tissue removal, retained more of the meniscus’s protective role. Their knees adapted through conservative management alone. The trial underscores how short-term gains from surgery may mask deeper, enduring drawbacks.
Shifting Advice for Patients and Clinicians
Orthopedic specialists now face pressure to reassess routine recommendations for meniscus tears. Physical therapy, weight management, and anti-inflammatory measures emerge as viable first-line options. Surgery should reserve for cases unresponsive to these approaches.
Patients benefit from discussing trial results with providers before consenting to procedures. Awareness of potential 10-year risks empowers informed choices.
- Prioritize structured rehabilitation programs early.
- Monitor symptoms closely before considering invasive steps.
- Seek second opinions on surgical necessity.
This study leaves orthopedic practice at a crossroads. For the millions annually diagnosed with meniscus issues, the message rings clear: preserving natural tissue might safeguard knees far longer than cutting it away. Future research will refine these insights, but patients today hold the power to weigh long-term health against immediate fixes.
