A racing heart, shortness of breath, a sudden wave of dread that seems to come from nowhere. For millions of people, a panic attack feels like a system failure happening in real time. The frustrating part has always been that there’s very little you can do once the spiral starts, at least that’s what most people assume.
That assumption is worth revisiting. A growing body of neurological research points to a small, cartilaginous flap on your outer ear, called the tragus, as a potential emergency off-switch for the fight-or-flight response. The science behind it connects ancient auricular medicine with modern neuromodulation, and it’s more credible than it might first sound.
The Scale of the Problem: Why Panic Management Matters Now

Anxiety disorders are the most common mental health disorders worldwide, yet only about one in four people with an anxiety disorder actually receive treatment for it, according to the World Health Organization. The treatment gap is striking. An estimated 359 million people around the world had anxiety in 2021, roughly four and a half percent of the global population.
Large-scale cross-national data from the World Mental Health Surveys found a lifetime prevalence of panic attacks at roughly thirteen percent, and among those who have ever experienced one, the majority go on to have recurrent attacks. That’s a very significant number of people cycling through crises with limited immediate tools to hand. The urgency to find fast, accessible interventions is real.
What the Vagus Nerve Actually Does
The vagus nerve is sometimes called the “wandering nerve” because it’s the longest nerve in the human body and travels from the base of the brain up into the ears and down into the lower intestines. It’s not just one nerve doing one job. It serves as a critical bidirectional communication pathway between the central nervous system and the autonomic nervous system, and anatomically it exhibits a unique fiber composition of eighty percent afferent and twenty percent efferent fibers.
The sympathetic nervous system owns the “fight or flight” response, preparing the body to respond to perceived threats by increasing heart rate and releasing stress hormones, while the parasympathetic nervous system is associated with the “rest and digest” response and helps the body return to calm. The vagus nerve plays a major role in promoting that relaxation, digestion, and recovery. When a panic attack strikes, the sympathetic system has essentially taken over. Stimulating the vagus nerve helps push back.
The Ear Connection: Why Your Tragus Is a Gateway
The auricular branch of the vagus nerve, also referred to as Arnold’s Nerve, arises from the superior ganglion, exits through the tympanomastoid suture of the temporal bone, and innervates the external tympanic membrane and a small portion of the posterior aspect of the external ear. This anatomical quirk is the entire basis of the ear-tapping technique.
The ear offers a pathway to the vagus nerve, making this part of the body a simple and accessible option to stimulate it in a non-invasive way. That vagus nerve ear connection is considered essential for health, so stimulating it can offer a range of benefits. The tragus, that small cartilage flap at the front of the ear canal, is particularly well-positioned for this. The cymba conchae may be innervated almost entirely by the auricular branch of the vagus, while the tragus also offers practical advantages in terms of applying stimulation to the anterior wall of the external ear canal.
What “Transcutaneous Auricular VNS” Actually Means

Transcutaneous auricular vagus nerve stimulation, or taVNS, has been investigated as a novel neuromodulation tool. In clinical settings, it involves electrodes placed on the skin of the ear. Through electrodes placed on the skin of the ear, over the tragus or cymba conchae, the vagus nerve transmits the impulse received from the taVNS device to stimulate various areas innervated by the vagus.
Vagus nerve stimulation via the external ear has been shown to increase the “relaxation response” of the parasympathetic nervous system and reduce fight-or-flight stress responses driven by the sympathetic nervous system. Manual tapping or firm pressure on the tragus region mimics this stimulation in a cruder but accessible form. The physiological pathway is the same, even if the intensity differs considerably from clinical devices.
The Brain Response: What Happens When You Activate the Vagus
Studies have shown that VNS can reduce anxiety among patients suffering from an elevated state of arousal associated with PTSD, and it is believed to trigger plasticity in brain areas such as the prefrontal cortex and amygdala, increasing acetylcholine and reducing stress and anxiety. These are precisely the brain regions that go into overdrive during a panic attack.
taVNS has been proposed to exert its effects by activating the cholinergic anti-inflammatory pathway, leading to the release of neurotransmitters such as acetylcholine and noradrenaline, which regulate autonomic tone and emotional states. It has also been demonstrated to influence cortical and subcortical brain regions implicated in anxiety regulation, such as the amygdala and prefrontal cortex. That chain of neural events is what produces the felt sense of calm. In healthy volunteers, taVNS reduces sympathetic stress markers, indicating that it shifts the autonomic balance toward parasympathetic dominance.
Research Support: What the Clinical Evidence Shows

A 2024 double-blind, randomized, controlled clinical trial published in Frontiers in Integrative Neuroscience found that transcutaneous auricular vagus nerve stimulation modulates masseter muscle activity, pain perception, and anxiety levels in university students. Importantly, the anxiety reductions were measurable. The researchers found that elevated anxiety levels correspond to heightened muscle tension and lower pain tolerance, and the mechanisms underlying these associations involve the autonomic nervous system’s response to stress, wherein heightened anxiety leads to increased sympathetic activity resulting in greater muscle tension.
Vagus nerve stimulation has been certified as an effective therapeutic modality for emotional disorders, especially anxiety triggered by post-traumatic stress disorder, and a 2025 study in Translational Psychiatry substantiated that taVNS significantly mitigates anxiety-like behaviors via activating specific glutamatergic neurons in the anterior cingulate cortex. The science is moving fast. taVNS has recently been shown to have effects in individuals suffering from various psychological conditions such as depression or anxiety.
How the Ear-Tapping Technique Is Practiced
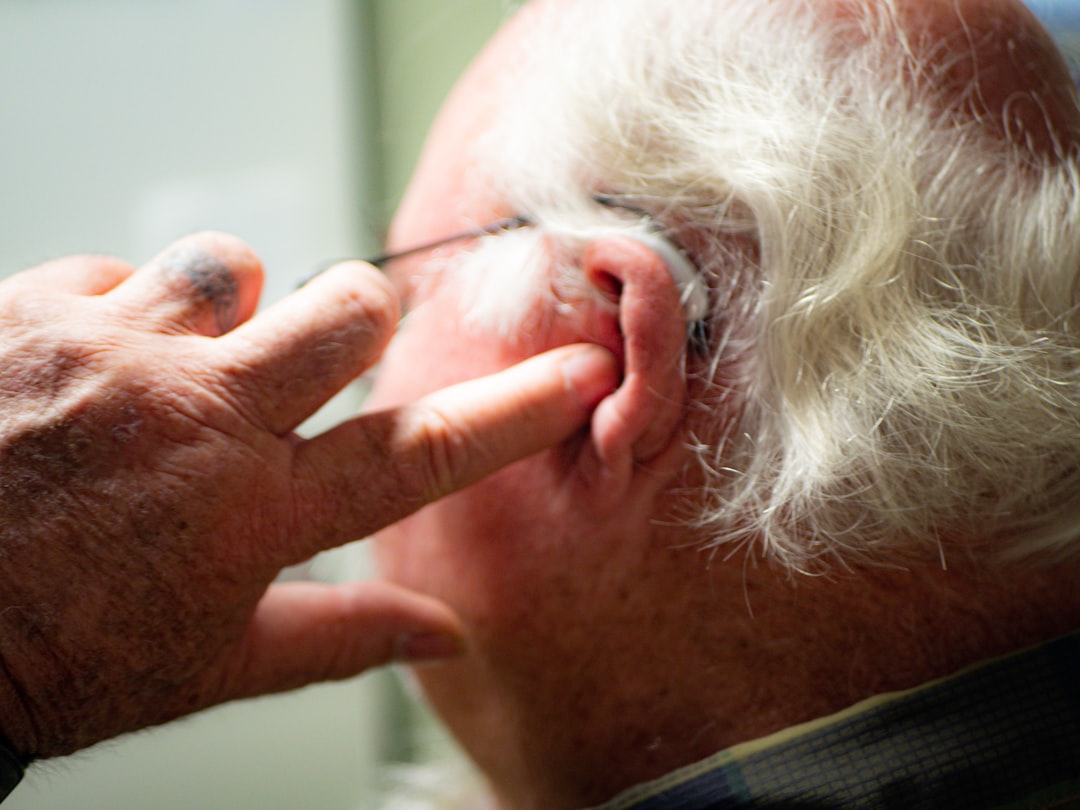
The manual version of this technique involves locating the tragus, the small pointed cartilage flap directly in front of the ear canal. Firm, rhythmic pressure or tapping is applied, typically with the index finger, for ten to thirty seconds. Ear massages increase blood flow and encourage the release of feel-good neurotransmitters in the brain, which further assists with relaxation.
Researchers have investigated the effects of auricular vagus nerve stimulation at the tragus for activating the parasympathetic nervous system to reduce stress. The manual approach is a simplified, tool-free approximation of what clinical taVNS devices do electronically. It doesn’t replicate the precision of clinical devices, but the anatomical target is the same, and some researchers suggest even mild mechanical stimulation of that nerve branch can produce a measurable parasympathetic signal.
Heart Rate Variability: The Measurable Signal of Calm

The impact of the vagus nerve on various bodily functions has been the subject of extensive research, leading to a better understanding of how vagal tone, a measure of vagus nerve activity, can affect the body. High vagal tone is associated with a lower resting heart rate, reduced blood pressure, and increased heart rate variability. Heart rate variability, or HRV, is increasingly used as a reliable physiological marker of nervous system state.
Transcutaneous auricular vagus nerve stimulation has been shown to increase heart rate variability during stimulation, based on electrocardiogram recordings. A rise in HRV is essentially the nervous system signaling that it’s shifting gears from threat mode to safety mode. Regular vagus nerve stimulation strengthens the vagal brake, which is the nervous system’s ability to quickly shift from stress to relaxation. That increased flexibility is what makes the technique useful over time, not just in the moment.
Important Limitations and What the Research Cannot Yet Claim

The honest picture requires some caution. The “ten seconds” framing in popular discussion of this technique is more aspirational than rigorously proven. Although taVNS is generally considered safe with only mild and transient adverse effects, clinical safety data from device-based studies is still being assembled. Manual tapping carries fewer risks than electrical stimulation, but it also produces a much weaker signal.
One 2025 study in Cognitive, Affective, and Behavioral Neuroscience found that taVNS did not influence physiological, psychological, or behavioral responses to an acute mental stressor, though the strong intercorrelation between sympathetic and parasympathetic indexes in the taVNS group suggests it does improve autonomic regulation in healthy participants. The evidence is promising but mixed, and results appear to vary by individual, baseline arousal state, and stimulation method. There is a recognized need for further research on the effectiveness of the different stimulation parameters used and the duration of treatments and sessions.
Where This Fits Alongside Conventional Treatment

Further studies have shown promising results that VNS can treat disorders such as anxiety disorder, Alzheimer’s disease, cluster headache, and heart failure, among others. This growing list of applications reflects just how central the vagus nerve is to systemic regulation. The ear-tapping technique, used in the context of panic management, fits into a broader framework of self-regulation tools. Research shows taVNS devices offer short-term and long-term symptom improvement for those with treatment-resistant anxiety disorders including panic disorder, though studies done with these populations have been small, meaning more research is needed. Early results are promising.
The potential advantages of taVNS include that it is designed specifically to address distressing stimuli and unresolved emotional memories, it is a brief and time-limited intervention, and its multi-modal design may appeal to and benefit a broader range of patients than a single-mode intervention. None of this replaces therapy, medication, or professional mental health support. It’s better understood as a practical, portable tool that can be used in the moment, sitting in a meeting, on the train, or anywhere else a panic response decides to arrive unannounced.
Conclusion

The science behind the vagus nerve and the ear is not speculative. It’s anatomically real, clinically explored, and increasingly supported by peer-reviewed research from institutions publishing in journals like Frontiers in Neuroscience, Translational Psychiatry, and Scientific Reports through 2024 and 2025. The exact mechanisms, the optimal pressure, the precise duration, and individual differences all remain open research questions.
What the evidence does support, carefully and without overstatement, is that the auricular branch of the vagus nerve is genuinely accessible through the outer ear, that stimulating it influences the autonomic nervous system’s balance, and that this influence can reduce anxiety-related arousal. Whether you tap with a finger or use a clinical device, you’re working with the same biology. That’s a meaningful place to start.


